|
Back to Blog
Spike protein5/25/2023 
What they found suggests “that individuals who developed myocarditis have a humoral immune response comparable to that of asymptomatic adolescents and young adults” who comprised the control group, the paper notes. The researchers tested for humoral and T-cell responses to SARS-CoV-2, antibody responses to common pathogens, cytokine levels, and SARS-CoV-2 antigens. Three-quarters developed myocarditis after their second dose, while the rest had their symptoms occur after the first (12.5%) and third (booster) dose (12.5%).Īn additional 45 age-matched individuals (average age 15 40% male) who were symptomatic up to 3 weeks after their second mRNA shot served as controls, also providing blood samples. Median time between vaccination and symptom onset was 4 days (range 1-19 days). Yonker et al analyzed blood samples from 16 patients ages 12 to 21 years (average age 16 81% male) who had been hospitalized between January 2021 and February 2022 at Massachusetts General Hospital for Children or Boston Children’s Hospital with myocarditis after receiving an mRNA-based COVID-19 vaccine.Īll presented with chest pain and elevated cardiac troponin T (median 260 ng/L IQR 215-1,114 ng/L) and C-reactive protein (median 29.75 mg/L IQR 15.53–50.58 mg/L). “The benefit of vaccination far exceeds any of these risks,” she said. “Even in the higher-risk group, which is age 16 to 30, it’s one in 20,000.” On the other hand, the incidence of myocarditis is “markedly higher” following COVID-19 infection than it is following vaccination, Bozkurt said, and people with the infection see increases in MI, stroke, arrhythmia, deep vein thrombosis, pulmonary embolism, and other cardiovascular events as well. Regardless of the mechanism, an important message is that myocarditis is extremely uncommon after mRNA vaccines, occurring at an incidence of around one to five cases per 100,000 in the general population, she emphasized. “Clearly, developing postvaccine myocarditis is much more rare than developing any of the complications of infection with SARS-CoV-2,” she noted.īiykem Bozkurt, MD, PhD (Baylor College of Medicine, Houston TX), who wrote an editorial accompanying the paper, said the study “is providing further information about the why and the how” of postvaccine myocarditis. What the results don’t do, she stressed, is change the fact that the data strongly support getting vaccinated against COVID-19. 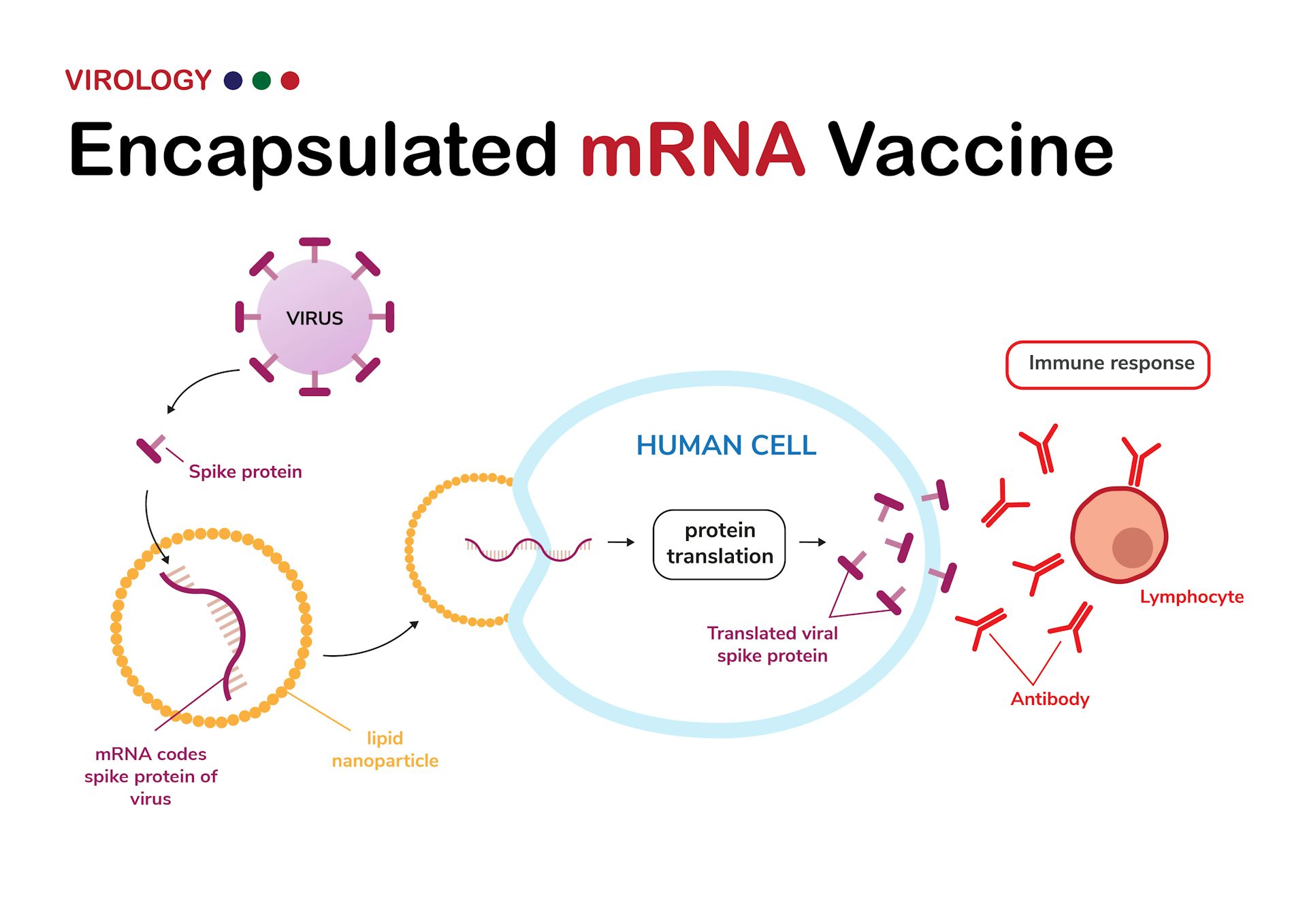 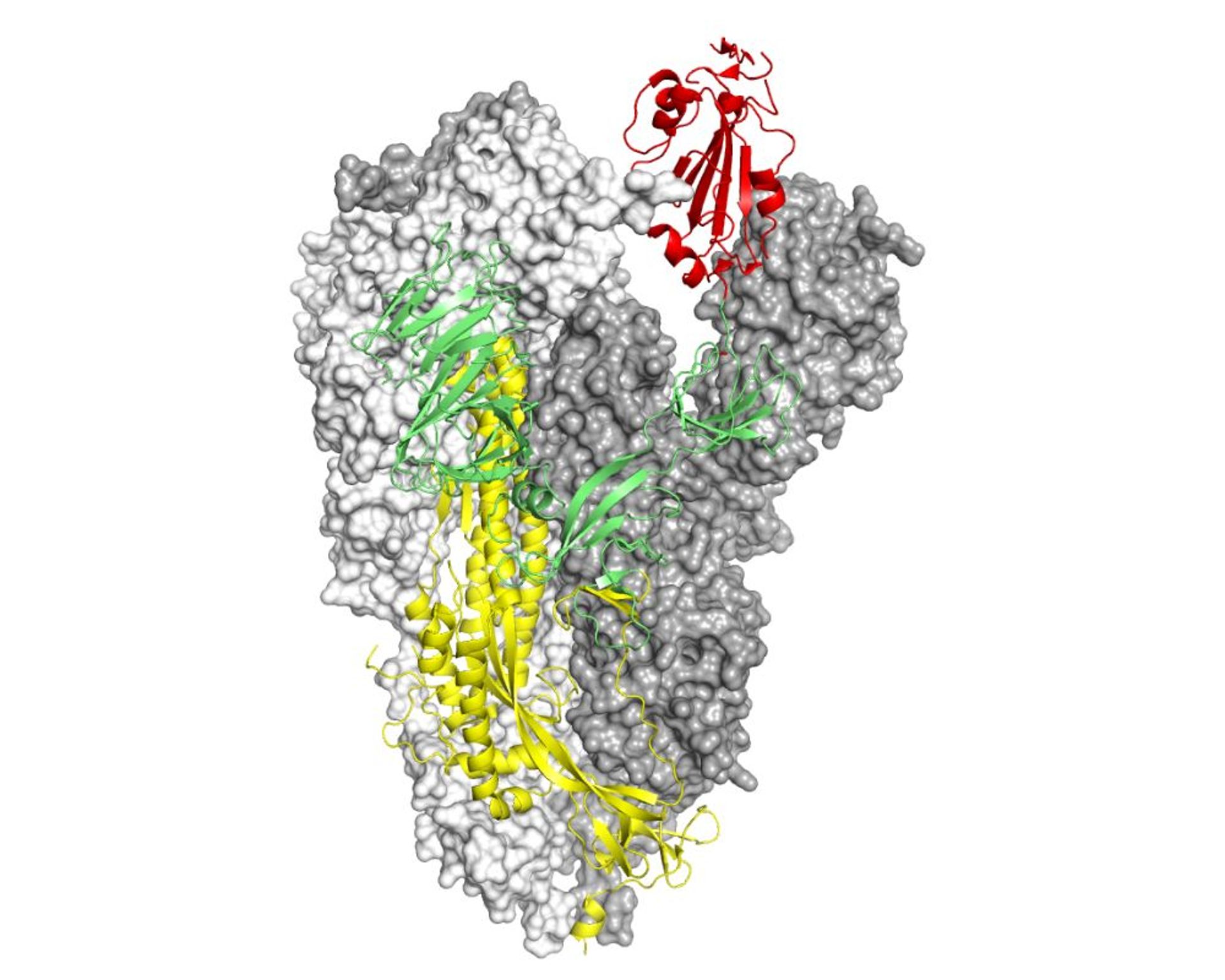
Exactly why individuals with myocarditis don’t clear it the same way isn’t yet known, said Yonker. Typically, though, these particles don’t stick around but get cleared as the body processes the vaccine. With myocarditis, the spike protein most likely arises downstream from the vaccine itself, not leftover virus, she explained. Lingering SARS-CoV-2 particles have been proposed as one mechanism for long COVID as well. Interestingly, said Yonker, a known feature of multisystem inflammatory syndrome in children (MIS-C), which can develop after the acute phase of COVID-19, is the persistence of viral particles in the body. We really didn’t see that at all, which surprised us,” she said. “We were expecting to see this hyper, revved up autoantibody response to the vaccine. Another possible idea had been that the mRNA COVID-19 shots trigger an overly vigorous immune response, thanks to either a genetic predisposition or testosterone. Yonker told TCTMD that, going into their study, the researchers had anticipated they would find a link between postvaccine myocarditis and autoantibodies that might be inadvertently targeting cardiac tissue. “We discovered that individuals who developed postvaccine myocarditis uniquely exhibit elevated levels of free spike protein in circulation, unbound by antispike antibodies, which appear to correlate with cardiac troponin T levels and innate immune activation with cytokine release,” they explain, adding, “Although these findings might provide insight into the immunophenotype of vaccine-related myocarditis, they do not alter the risk-benefit ratio strongly favoring vaccination to protect against severe COVID-19-related complications.” Yonker, MD (Massachusetts General Hospital, Boston), and colleagues turned to immunoprofiling as a way to better understand the underlying mechanisms. Prior studies have provided insight into the key clinical features of myocarditis cases, rare but real, seen with Pfizer/BioNTech’s BNT162b2 and Moderna’s mRNA-1273 vaccines.įor their paper, published online in Circulation, Lael M. Levels of the antigen were unusually high among those with myocarditis. Instead, the complication seems related to how some individuals process spike protein, produced by the body using the vaccine’s mRNA as a template. Myocarditis that arises after receipt of an mRNA-based COVID-19 vaccine among adolescents and young adults does not appear to result from a heightened overall immune response or from autoantibodies, new data suggest.
0 Comments
Read More
Leave a Reply. |
 RSS Feed
RSS Feed
